“The Quality of Mercy:” Tredwell Philanthropy, Part 2
by Ann Haddad
The Tredwells’ Good Genes
Between 1821 and 1840, Seabury Tredwell’s wife, Eliza, gave birth to eight children. Considering the primitive medical care available in the antebellum period, and the resulting high rate of infant and childhood mortality, it is remarkable all of the Tredwell children lived to adulthood. Gratitude for their good fortune in light of the risks associated with childbirth may have been the impetus behind the Tredwells’ decision to support the New York Asylum for Lying-In Women (NYALIW).
Poor, Widowed, Abandoned Women
By the turn of the 19th century, many women found themselves struggling alone to support themselves and their children. Two major yellow fever epidemics, in 1795 and 1798, left many of them widowed. The influx of immigrants to New York City led to a population boom, but jobs were scarce for this group.
| . |
Husbands frequently needed to travel far from the city in search of employment. Some never returned. The incidence of alcoholism among the poor increased. As a result, many pregnant women lacked traditional family support, especially when assistance was needed as the time of their confinement approached.
It is ironic that, although America began to take on a sentimental attitude toward motherhood in the late 18th century, moralistic and religious convictions found many pregnant women, especially unwed ones, with no other recourse for medical care except the almshouse at Bellevue Hospital. “Respectable” women sought to avoid this institution, however, as it had a reputation for being a haven for prostitutes and other “degraded” women.
Wealthy Women to the Rescue
In the early 1820s, wealthy women began to focus their reform efforts on women’s causes, such as education and improved health care. In 1823, a group of benevolent women led by Mrs. Arthur Tappan, wife of the abolitionist Arthur Tappan, established the New York Asylum for Lying-In Women. Its aim was to provide temporary accommodations and skilled medical assistance to poor but “reputable” women during their confinement. “Reputable” in this case meant married; in fact, all applicants were screened by a committee, and were required to furnish a marriage certificate and character references to be considered for admission.
Once admitted, a woman was supplied with a bible and a list of rules, which stipulated that she could not leave the building, could not receive visitors, and could not remain longer than four weeks after delivery. Alcohol was forbidden; that which was used for medicinal purposes was kept in a locked cabinet. Emphasis was placed on order, morals, and obedience. To emphasize their noble mission, the board of the NYALIW included the following passage from William Shakespeare’s The Merchant of Venice in their first Annual Report:
“The quality of mercy is not strain’d.
It droppeth as the gentle rain from Heaven
Upon the place beneath: It is twice blest;
It blesseth him that gives and him that takes.”
By Women, for Women
Although it employed a resident male physician, the NYALIW was unique in that it was managed and run by women: it had an all-female board, and barred male medical students from entering the institution. Births were attended by either a midwife or the matron. Postpartum care and vaccination of all newborns against smallpox were provided before discharge.
The charity’s first home was the Square Ward of New York Hospital, then located on Broadway between Anthony Street (now Duane Street) and Catherine Street (now Worth Street), which opened for admissions on November 1, 1823. The first patient was Catherine Martin, the wife of a weaver, John G. Martin, who had left his wife three months previous to look for work. Mrs. Martin was admitted on the 21st of November, and gave birth to a healthy child. She was discharged on January 1, 1824.
The Tredwells Support NYALIW
Within a few years the NYALIW outgrew its ward at New York Hospital, and sought donations for the purchase of larger quarters. In 1825, Seabury Tredwell was among the first group of donors, giving $24; the amount collected enabled the charity to move to larger facilities on Greene Street. In 1830, the charity had garnered sufficient funds to relocate to a three story building on 83 Marion Street (now Lafayette Street), where it remained until its move in 1885 to 139 Second Avenue, between 8th and 9th Streets, in the heart of the 14th Ward.
In 1832, Seabury once again donated to the NYALIW. His $25 subscription made him an “Honorable Member for Life,” along with other prominent citizens such as Joseph Brewster, Philip Hone, Duncan Phyfe, and Benjamin and George W. Strong. No doubt the Tredwells felt strongly about this cause, because from 1828 to 1861 Eliza Tredwell, an Annual Subscriber, donated $3-$5/year.
As a Subscriber, Seabury was permitted to recommend two women per year to the institution. One supporter who wrote a letter of recommendation for a woman in need was John J. Connor, who wrote the following:
“The bearer Ann Brennen whose husband is a poor laborer and unable to provide now for her is an honest and reputable person and I therefore recommend her to the humanity of the Managers of the N.Y. Asylum for Lying in women.
Mulberry 263. John J. Connor
Saturday March 8th 1834″
.
Heartbreaking Stories
One story in the NYALIW’s minutes, which is typical of the circumstances that befell many poor women, is that of Mrs. Anne Croaker, who applied for admission on September 13, 1828. Her husband, who had worked as a locksmith for seven years for a Mr. Pye, had recently died. His death was hastened by a dose of arsenic, which was sold in error by the druggist. Mrs. Croaker, left completely destitute, lived with her five young children in a room on Canal Street, which had been loaned by a friend. The Admissions Committee visited Mr. Pye, who vouched for Mrs. Croaker’s character; he stated that she was forced to “sell her most valuable things to procure comforts for him [Mr. Croaker] during his illness.” Mr. Pye generously offered to provide for the children during their mother’s confinement.
Women seeking relief came from Connecticut, Pennsylvania, and outlying parts of New York State. Mrs. Collin Reed, a wealthy New Yorker who served on the Admissions Committee for NYALIW in 1824 and 1825, noted the following in her ledger book:
“Received in the lying-in Ward Eliza Robinson of Connecticut, Litchfield. In case of her death, her infant is to be sent to her friend. [Eliza is] clean and tidy, but very destitute. She supports herself by taking work from the slop shops. Received on the 18th of May, left June 6th.”
In 1831, due to the insufficient numbers of married women who were seeking assistance at the doors of NYALIW, the institution broadened its admission requirements to include unmarried women. It also began making home visits to extend its outreach. For several years previous, however, some committee members had begun to overlook the questionable tales of woe and the dubious marriage certificates furnished by some applicants; thus a number of unmarried women were permitted to enter.
NYALIW’s Employment Agency
| . |
Upon their discharge, the administration sought to place unmarried women as wet nurses in respectable families for one-year periods. After careful screening at the time of admission, observation throughout their confinement, and physical examination by a physician at the time of delivery, the charity was able to offer a guarantee of the health and character of the wet nurses hired by prospective upper class families. In 1828, NYALIW proudly announced that “Of fifty who have been discharged from the house…23 have obtained places as wet nurses in respectable families.” No mention was made of the fact, however, that these women most likely would have had to find a wet nurse for their own infants.
At its 48th annual meeting, held on April 19, 1871, NYALIW reported that since opening its doors, it had gratuitously assisted 16,329 women. It noted that in 1870, 86 patients had been treated at the Asylum, and 188 more at their homes.
In 1894, NYASIW changed its name to the Old Marion Street Maternity Hospital; in 1899, it merged with the New York Infant Asylum. The charity ultimately became the Obstetrics and Gynecology Department of New York Hospital-Cornell Medical Center.
A Christmas Recipe from 1825
Like many 19th century women, Mrs. Reed, NYALIW’s Admission Committee Member, used her manuscript ledger as a recipe book as well as a diary and account book. Here is her recipe for a festive “Rich Plum Cake”:
Of flour, butter and sugar 3 pounds each, 2 doz eggs, 4 lb and a half of currents 6 lb of raisins, mace, cinnamon, nutmeg each ounce 1/4 oz of cloves, 2 tablespoon full of ginger 2 gills of wine, 1/2 pound of citron.
Wishing you a joyous holiday season! Merry Christmas!
Sources:
- “Anniversary of the New-York Asylum for Lying-In Women.” New York Times. April 20th, 1871, p. 2. timesmachine.nytimes.com. Accessed 12/6/16.
- Burrows, Edwin G. and Mike Wallace. Gotham: A History of New York City to 1898. New York: Oxford University Press, 1999.
- Golden, Janet. A Social History of Wet Nursing in America: From Breast to Bottle. Cambridge, U.K.: Cambridge University Press, 1996.
- Managers of the New York Asylum for Lying-In Women. Annual Reports, 1824-1855. www.archive.org Accessed 11/15/16.
- Minutes, 1823 Nov. 1-1831 Feb. 28. New York Asylum for Lying In Women. BV 89584. New York Historical Society Manuscript Collection.
- New York Asylum for Lying-In Women Materials. Delaplaine Family Papers. 89638. Box 4, Folder 9. New York Historical Society Manuscript Collection.
- Quiroga, Virginia A. Metaxas. Poor Mothers and Babies: A Social History of Childbirth and Child Care in Nineteenth Century New York City. New York: Garland Publishing, Inc., 1989.
- Shakespeare, William. The Merchant of Venice, Act IV, Scene 1.
The Doctor in the House is a Homeopath!
by Ann Haddad
A Discovery in the Archives
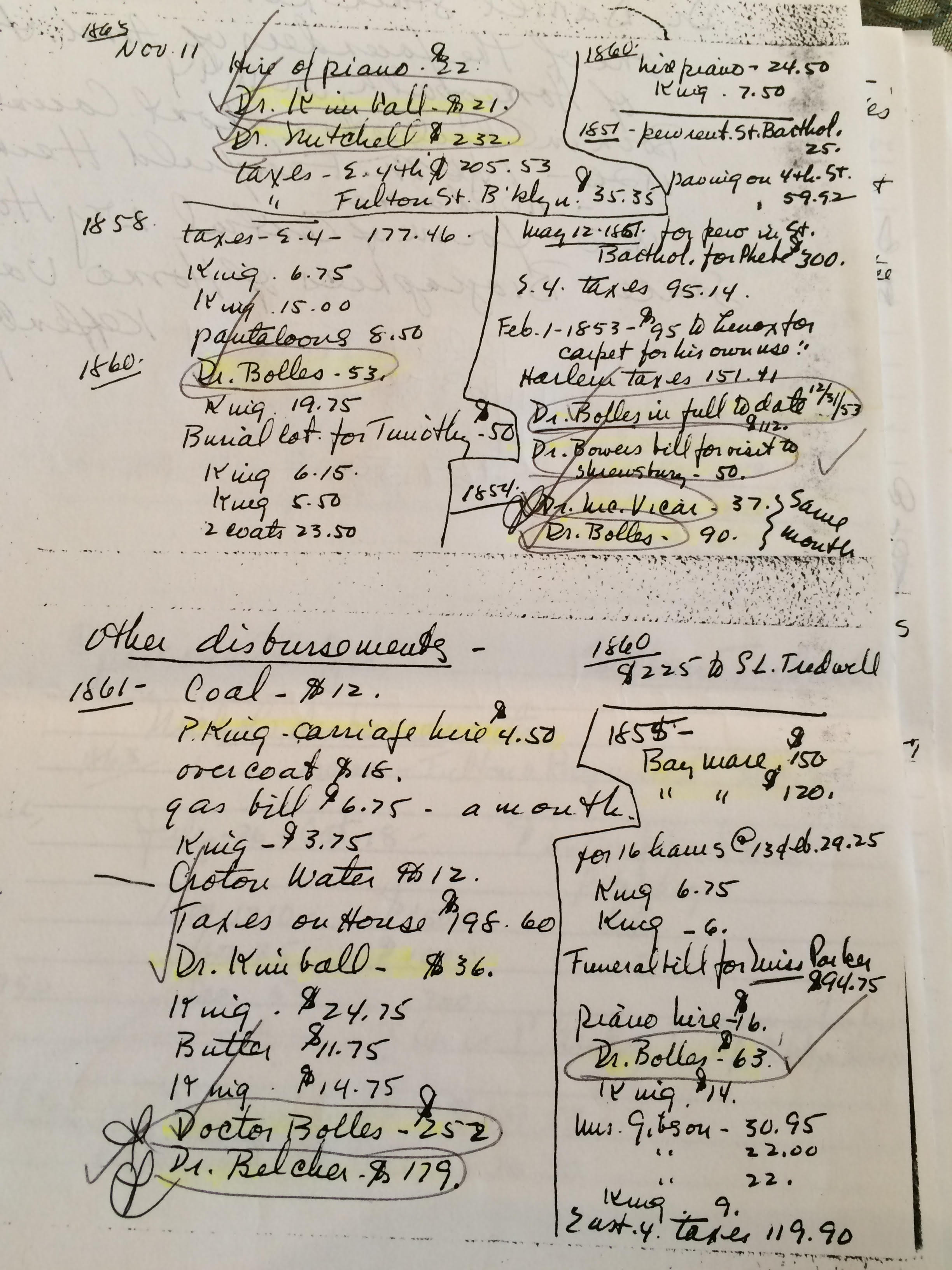
Among the papers in the Tredwell family archives are notes, copied by a staff member from Seabury Tredwell’s personal ledger, that date from 1851 until his death in 1865. (Unfortunately, the ledger is missing.) Judging by his detailed entries of monthly debits and credits, Seabury kept a tight hold on his family’s purse strings. He carefully included expenses both large and small, such as his pew rental at St. Bartholemew’s Church in 1851 ($300), frequent carriage rentals ($8 average), and 16 hams ($29.25).
The most exciting information gleaned from Seabury’s ledger book, however, relates to payments to various physicians for 18 house calls made during those 14 years. Based on standard medical practice of the time, that would have meant a lot of purging and bloodletting. But most likely, not a drop of blood was shed in the Tredwell household in the name of therapy; for in researching the medical practices of the six doctors who ministered to the Tredwell family, it was discovered that, far from being mainstream practitioners, they were all non-traditional homeopaths.
The Typical Treatment: Arsenic and Leeches
Prior to the development and gradual acceptance of germ theory in the mid-to-late 19th century, summoning one’s physician to treat an illness was risky at best. Orthodox medical practice offered little in the way of treatments, and the choices were harsh, potentially toxic and painful, and largely futile. Mercury, arsenic, and lead were used to elicit violent purging and vomiting; bloodletting and use of leeches caused severe anemia, which only worsened the patient’s condition. As a result, laymen developed a severe distrust of physicians, and expressed their doubts and criticisms publicly.
The Emergence of Homeopathy
| . |
As “regular” physicians (or allopaths) struggled to identify more evidence-based treatment modalities, homeopathy emerged as a sophisticated and gentler alternative to the barbaric practices of regular medicine. The origin of homeopathy dates to the work of the German physician Samuel Hahnemann (1755-1843). It was introduced in the United States by Hans Burch Gram (1786-1840), who began practicing medicine in New York City in 1825. Treatment was based on the “Laws of Infinitesimal Dose” and the “Law of Similars,” in which minute and extremely diluted doses of medicines were administered to produce symptoms similar to those of the disease being treated, thereby allowing the body to naturally heal. This was perceived as a gentler, more holistic approach to treating disease.
The recovery rates of patients treated with homeopathy were higher than those treated by orthodox medicine, simply because the new remedies did little or nothing to harm the patients. The apparent success of this new approach, especially during the cholera epidemic of 1832, led many regular physicians to seriously consider “converting” to more homeopathic remedies. Many of these were physicians who had trained at highly regarded allopathic medical schools.
.
The Practice Grows
In 1834-1835, both the New York Homoeopathic Society and The American Journal of Homoeopathia were established. By 1844, the number of practicing homeopaths in the United States had grown to such an extent that the American Institute of Homeopathy was formed. In 1860, the Homoeopathic Medical College of New York was opened and by 1900, the city had more than 100 homeopathic hospitals, clinics, and dispensaries, including one on Bond Street, two blocks away from the Tredwells’ home.
If Mark Twain Believes in It …
Many highly respected public figures of the day espoused the benefits of homeopathy, thereby contributing to its increasing popularity. Henry Wadsworth Longfellow, William Cullen Bryant, Daniel Webster, and Henry James were advocates of its methods. Homeopathy was also very popular among women, including authors Harriet Beecher Stowe and Louisa May Alcott, and members of the clergy. Mark Twain, another believer, said in 1890 that homeopathy:
“…Forced the old school doctor to stir around and learn something of a rational nature about his business, … And you may honestly feel grateful that homeopathy survived the attempts of the allopaths to destroy it.”
The number of homeopaths in New York City grew from 93 in 1857 to 322 in 1904, which was over 15 percent of all practicing physicians.
Traditional Medicine vs. “Quackery”
The reaction by the majority of mainstream physicians and pharmacists to the new practice of homeopathy was fierce and prolonged. Labeled as “quacks” and “irregulars,” homeopaths were perceived as a threat to the medical establishment, for financial as well as theoretical reasons. The traditional physicians were losing patients, and the apothecaries lost business, because homeopaths typically prescribed one medication at a time, and in minute doses. In 1847, the established members of the New York medical community united against the practice of homeopathy and formed the New York Academy of Medicine, and on February 3rd of that year, the first President of the Academy, Dr. John Stearns, had this to say about homeopathy in his inaugural address:
“No man in the full exercise of his reason can believe in the truth of this strange doctrine; and if he attempts to practice upon the principles which that doctrine inculcates, he must possess a depraved moral faculty.”
That same year, the American Medical Association was founded, largely to impose severe restrictions on all forms of alternative medicine. The battle of the allopaths and the homeopaths was fought in the newspapers. The following anonymous poem, which appeared in the Brooklyn Daily Eagle in November 1849, lambasts the heavily diluted therapies prescribed by homeopaths:
“Take a little rum,
The less you take the better,
Mix it with the lakes
Of Wenner and of Wetter.
Dip a spoonful out–
Mind you don’t get groggy–
Pour it in the lake
Winnippisseogee.
Stir the mixture well,
Lest it prove inferior;
Then, put a half a drop
Into Lake Superior.
Every other day
Take a drop of water;
You’ll be better soon,
Or at least you ought to.”
Seabury Tredwell Meets Homeopathy
We do not know why or when Seabury Tredwell began to turn to homeopaths for his family’s medical care. There were at least four physicians in his immediate and extended family; although the nature of their practices is unknown, they were most likely allopaths. Seabury may have been influenced by colleagues in the mercantile world, two of whom, Robert B. Folger and Ferdinand Little Wilsey, studied homeopathy and established medical practices after being successfully treated by Dr. Gram in 1826.
| . |
Who Were These Guys?
Whatever his motivation, records indicate that between 1853 and 1865, Seabury relied exclusively on homeopathic physicians. Dr. Richard M. Bolles (1797-1865), made the most frequent house calls to the Tredwell family between 1853 and 1861. He adopted the tenets of homeopathy in 1840, and his practice diminished as a consequence. Bolles remained an advocate of this alternative treatment, and served as president of the Hahnemann Academy of Medicine. He also worked in several of the homeopathic dispensaries in the city. His Poetic Descriptions of the Chest-Pains and their Appropriate Remedies was famous among homeopaths. Dr. Bolles’ bills to the Tredwell family over eight years totaled $693. He died in August 1865, five months after the death of his patient, Seabury Tredwell.
Dr. Benjamin F. Bowers (1796-1875), who was considered very influential on the growth of homeopathy in New York, made one visit in 1853 to the Tredwells’ farm in Rumson, New Jersey. Dr. Bowers was expelled from his position at the New York Dispensary in 1839 for providing non-traditional medical care. He later served as president of the Homeopathic Medical Society of New-York, and was involved with the Protestant Half-Orphan Asylum (as was his colleague Dr. Bolles, who served as Medical Supervisor), a charitable institution that:
“… has been exclusively under homeopathic treatment for the past 24 years with the most gratifying results, having had an average mortality as compared with all the other asylums in the city, of only one to three.”
Dr. George Belcher (1818-1890), who ministered to Seabury Tredwell during his final illness in March 1865 (Dr. Bolles having retired some years prior), had one of the largest medical practices in New York City. An 1839 graduate of Columbia College of Physicians and Surgeons, he “converted” to homeopathy in 1844. He signed Seabury Tredwell’s death certificate, listing Bright’s Disease (now nephritis, or kidney disease), as the cause of death. On December 31, 1865, he submitted his bill for $70 for his final visit to the Tredwell home on East 4th Street.
Following in Father’s Footsteps
After his death in 1865, at least one of Seabury’s children continued to turn to homeopaths for medical treatment. Elizabeth Tredwell Nichols (1821-1880), Seabury’s oldest child, was a patient of Dr. John Samuel Bassett (1830-1912), a Harvard-trained physician with a practice on West 31st Street, near the Nichols’ residence on Fifth Avenue and 34th Street. Dr. Bassett was a highly regarded physician to many of New York City’s most distinguished families, including the Astors, Chandlers, and Rhinelanders. A respected member of the American Institute of Homeopathy, Dr. Bassett was frequently consulted by other physicians because of his skills as a diagnostician. In 1880, he attended Elizabeth in her final struggle with chronic bronchitis. Elizabeth was 59 years old at the time of her death.
Demise, Then Resurgence
After the turn of the century, the popularity of homeopathy gradually declined as a result of the increasingly scientific approach and rational treatments of regular medicine. By 1923, only two homeopathic colleges remained in the United States, and by 1950 they too had closed.
Within the past 40 years, homeopathic medicine has re-emerged onto the medical scene. It is not unusual for mainstream physicians who focus on a holistic approach to patient care to incorporate homeopathy in their practices, and homeopathic remedies are sold in pharmacies alongside traditional medicine. The Tredwells, no doubt, would feel perfectly at home.
Sources:
- Bowers, Benjamin F. “Opposition to Homeopathy in New York,” in The North American Journal of Homeopathy. Vol. 15, May, 1867, p 580-604. http://books.google.com. Accessed 9/26/16.
- Bradford, Thomas Lindsley. Biographies of Homeopathic Physicians, Vols. 3, 4, 19, 21, 22: Beach-Bixby. Philadelphia, 1916. www.archives.com. Accessed 9/22/16.
- Brooklyn Daily Eagle. Friday, November 9, 1849. www.newspapers.com. Accessed 9/30/16.
- Duffy, John. History of Public Health in New York City, 1625-1866, Volume 1. New York: Russell Sage Foundation, 1968. p. 464-471.
- “Homeopathic Directory.” New England Medical Gazette. April, 1871, p. 190-191. www.archive.org. Accessed 9/8/16.
- King, William Harvey, Ed. History of Homeopathy and Its Institutions in America. New York: Lewis Publishing Co., 1905. www.archive.org Accessed 9/28/16.
- Starr, Paul. The Social Transformation of American Medicine. New York: Basic, 1982.
Ullman, Dana. A Condensed History of Homeopathy. www.homeopathic.com. Accessed 2/28/16.
Julia Tredwell Takes the “Water-Cure”
by Ann Haddad
 Julia Eliza Tredwell (pictured at right), Seabury and Eliza’s sixth child, was born on May 16, 1833. She was two years old when her father purchased the house on East Fourth Street that would be Julia’s home for the rest of her life. Many books in the Tredwell Book Collection bear her name, including several on French language and grammar, natural history, poetry, and mathematics.
Julia Eliza Tredwell (pictured at right), Seabury and Eliza’s sixth child, was born on May 16, 1833. She was two years old when her father purchased the house on East Fourth Street that would be Julia’s home for the rest of her life. Many books in the Tredwell Book Collection bear her name, including several on French language and grammar, natural history, poetry, and mathematics.
Julia’s Mysterious Illness
In a letter in the museum’s archive, written in August of an unnamed year, Julia expressed her concerns about her health to her mother. She was a guest at the National Hotel in Richfield Springs, a popular spa resort town in upstate New York, where she apparently went to take the “water-cure” to recover from an illness.
“I have felt very much better the past week. They all say I have gained. I feel it, but by weight I only have gained two pounds. I took a bath and I felt stronger as soon as I came out … It is so lonesome to be separated that I feel as if I ought not to stay as long as I have, but I hope in so doing that I will quite gain my strength.”
An Ancient Health Remedy: Water
Although we do not know the nature of the illness that befell Julia that summer, it would certainly not have been unusual for her to seek treatment at a spa hotel that offered the “water-cure,” a 19th century health reform movement that employed the therapeutic use of water to revitalize health and treat disease. Also known as hydrotherapy, it has been practiced since ancient times, when Greeks, Romans, and other early civilizations employed water for medicinal purposes. The perceived therapeutic value of springs rich in minerals such as bromine and sulfur was thought to be attained by a combination of bathing and drinking the water. After waning in the Middle Ages, the popularity of this form of alternative medicine spread throughout Europe and eventually became a craze in the United States, in part as a reaction to the brutal practices of blood-letting, purging, blistering, and other medical treatments of the time, which often worsened the patient’s condition.
The “water-cure” involved various rituals, some less aggressive than others, such as submersion in hot or cold tubs of mineral-rich water for hours at a time; wrapping in cold sheets and then sweating; as well as ingestion of 1-2 liters of foul-tasting mineral water in one sitting. Cold water enema was also considered to be of therapeutic value in treating bowel inflammations and constipation. The “water-cure” was prescribed for the relief of many other ailments, especially gout and arthritis; it offered a gentler alternative to the violent medical therapies typically employed. Dietary remedies, including abstention from coffee, tea, salt, and alcohol, as well as meat and dairy products, were also prescribed.
“For the Invalid and Pleasure Seeker”: Water-Cure and Vacation in One!
By the mid-19th century, the popularity of summer resort towns built around curative springs had soared, especially in New York State. The grand spa hotels typically featured hot and cold water therapy along with dietary and hygienic programs. Ever fearful of the summer cholera and other illnesses caused by the “miasma” that pervaded the air in New York City, those wealthy enough to escape eagerly adopted this fashionable practice, combining their quest for health with a desire for an elite vacation amidst splendid scenery. Among the most popular spa towns were Saratoga Springs, Ballston Spa, and Richfield Springs, which was celebrated for its sulfur water. Located about 65 miles west of Albany, Richfield Springs, where Julia stayed one August, began to draw visitors as early as the 1820s, after Dr. Horace Manley brought 25 patients to take the “water-cure” at his new sanitarium on the site of the Great White Sulphur Springs.
The Water-Cure for New Yorkers, Too
In 1843, Dr. Joel Shew (1816-1865) established a hydropathic treatment business in New York City, the first of its kind in America. He and his wife, Marie Louise Shew, ran the center out of their home on 4th Street, four blocks away from the Tredwell home. In 1845, Dr. Shew founded “The Water-Cure Journal and Herald of Reforms,” which promoted the principles and efficacy of the “water-cure.” Mrs. Shew, herself a staunch promoter of healthy living for women and children, wrote a popular treatise on the benefits of the water-cure, as well as proper diet and exercise, “Water-Cure for Ladies.”
By 1846, the Shews had relocated to 56 Bond Street, just a block from the Tredwells, where their Institution for the Practice of Water-Cure, was “situated in a very airy and pleasant part of up town, New York.” The Shews charged $1 to $2 per day for room and board, medical treatment, and advice, and focused their attention particularly on lung disorders, as “the air of New York is exceedingly bland and favorable for cases of the above-named kind.” The Tredwells may have known of the Shews’ water-cure business; they most likely would have been acquainted with and perhaps even subscribed to the Journal, as it was a very popular periodical of the time, acquiring 50,000 subscribers by 1850. As Dr. Shew stated in his Water-Cure and Health Almanac of 1847:
“…by the judicious use of cold water alone, the good effects of bleeding and blistering are most readily produced, without any of the bad effects, including the pain.”
Mineral Water in Central Park
Even New York City residents who did not have the means to escape the heat and humidity of their home town had access to therapeutic waters. In 1869 Central Park opened its own Mineral Water Pavilion north of the Sheep Meadow, which sold many varieties of spring water with desirable chemical properties thought to promote health and cure illness. Not to be outdone by the offerings of the lavish summer resorts outside of New York City, the Pavilion offered morning summer recitals as an entertainment for the water-ingesting masses. Due to the unprecedented demand for mineral water in the city, merchants in the spa towns took to bottling the mineral water and shipping it to the municipal markets. In the letter to her mother, Julia refers to a neighbor being able to obtain the mineral water from “Cozzens,” who is mentioned in an advertisement in The New York Times, May 16, 1861:
“Sulphur water from these celebrated Springs has been kept for sale, at F.S. Cozzens, number 23 Warren Street.”
Did Julia Recover?
By the turn of the century, with the discovery of germ theory and advances in drug therapy, and as the leisure class sought other forms of entertainment, the popularity of the resort spa towns and the “water-cure” declined. While we don’t know if the “water-cure” proved therapeutic for Julia, or if that was her only foray into a spa town for her health, it most likely did her no harm. She died in 1909 at her home on East 4th Street, at the age of 76.
Sources:
- Bailey, W.T. Richfield Springs and Vicinity. New York: A.S. Barnes & Co., 1874.
- Legan, Marshall Scott. Hydrotherapy, or the Water-Cure in Wrobel, Arthur, ed. Pseudoscience & Society in 19th-Century America. Lexington: The University Press of Kentucky, 1987.
- Miller, Tom. “The Lost Mineral Water Pavilion of Central Park.” Web blog post. Daytonian in Manhattan daytoninmanhattan.blogspot.com. 14 August 2010. Web 20 April 2016.
- Shew, Joel, ed. Water-Cure and Health Almanac for 1847. New York: William H. Graham, 1846.







![Henry Monnier. “Allopath and Homeopath argue over method of treatment. [183-]”. (National Library of Medicine.)](https://merchantshouse.org/wp-content/uploads/2016/10/allopath-argue.jpg)








